This is a summary of my notes and I remember there were multiple choice questions about these enzymes on the exam.
Amino Transferases
Aspartate: AST
Alanine: ALT (more specific than AST)
Both enzymes are widely distributed in tissues but ALT is only present in small amounts except in the liver. There are no tissue specific isoenzymes.
Increased plasma levels of AST are characteristic of hepatocellular damage but can also be caused by:
pancreatitis
skeletal muscle disease
myocardial infarction
surgery/trauma
Plasma ALT is raised to a similar extent than AST in liver diseases but not in the other diseases
Alkaline Phosphatase (ALP)
ALP is present at high concentration in the liver, bone (osteoclasts), placenta and intestinal epithelium. These tissues contain specific isoforms of ALP which will help determine the tissue of origin. Thus measurement of ALP isoforms will distinguish between hepatic, osseous or other diseases.
Increased level of ALP is characteristic of cholestasis /biliary obstruction. The increased level in cholestasis is due to an increase in enzyme synthesis. Therefore, the levels of ALP, as well as GGT, will “peak” later than the levels of AST/ALT.
Gamma Glutamyl Transferase (GGT)
GGT is present at high concentration in the liver, kidney and pancreas but not in bone.
It is high in patients with alcoholic liver disease.
This enzyme is a very sensitive indicator of liver diseases as it is found in both cholestasis and hepatocellular damage.
Albumin
The most abundant plasma protein, is synthesised in the liver.
Because of its long half-life in the plasma, its concentration is normal in acute hepatitis but tends to decrease in chronic liver disease, partly due to decreased synthesis.
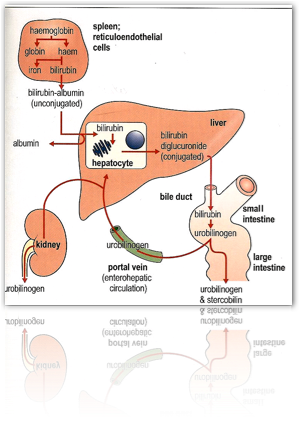
Bilirubin
The breakdown product of haem. The major sites of biosynthesis of haem are the liver and the erythrocyte-producing cells of the bone marrow which are active in haemoglobin synthesis.
Degradation occurs in the liver and spleen.
The diagram below shows you the different steps in the metabolism of bilirubin.
Reviewing My Notes
14th January